Complications of Spinal Muscular Atrophy: Scoliosis
Reviewed by: HU Medical Review Board | Last reviewed: August 2021 | Last updated: April 2024
People with spinal muscular atrophy (SMA) experience muscle weakness that gets worse over time (progressive) because of defective motor neurons. In severe types of SMA, progressive weakness can cause serious complications. One of the most common complications of SMA is spinal deformity, such as scoliosis.
Scoliosis is an abnormal spine curvature caused by back muscle weakness. Nearly all people with types 1 and 2 SMA develop scoliosis, as well as many people with type 3 SMA. It can impair mobility and lead to breathing difficulties. Physical therapy and bracing are focused on delaying scoliosis or slowing progression. Severe scoliosis may require treatment with spine surgery.
What is scoliosis?
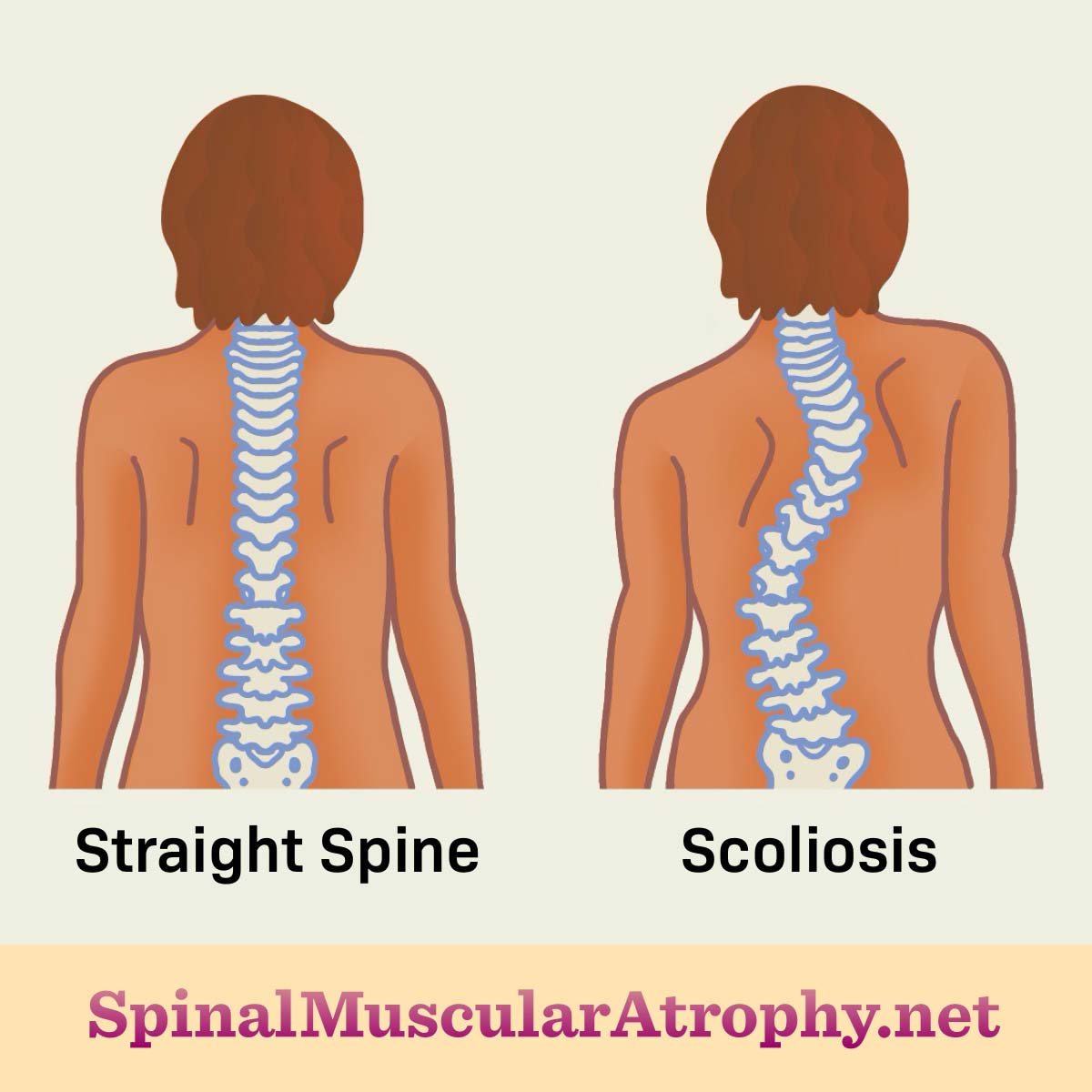
Scoliosis is a progressive curvature of the spine. It usually refers to a sideways “S-shaped” curve. Other types of spine deformities are also common in SMA, including an outward-bending “C-shaped" curve (kyphosis).1,2
Scoliosis reduces mobility and causes joints to stiffen or displace. Joints placed under stress by the spine are especially disturbed, such as the hip. This can lead to unstable sitting and impaired daily activities. Combined with respiratory muscle weakness, it can also cause breathing difficulties. This is because the curved spine restricts how much space the lungs have to expand and hold air. This is called restrictive lung disease.2,3
Figure 1. A normal spine compared to a spine with scoliosis
Why does spinal muscular atrophy cause scoliosis?
Scoliosis is one of the most common complications for people with SMA. It happens when back muscles that support the spine progressively weaken. These muscles receive signals from the brain through motor neurons in the spine. However, people with SMA have a genetic mutation that causes these motor neurons to die. Without signals from the brain, back muscles begin to weaken and waste away.4
People with type 1 and 2 SMA have a very high chance of developing scoliosis. Between 60 to 90 percent of children with type 1 and 2 experience it. People with type 3 SMA who cannot walk may also develop scoliosis.5
What are the symptoms?
Scoliosis is often diagnosed at an early age in people with SMA. In type 2 SMA, it can appear before age 4. Most cases of scoliosis appear before age 10. It usually progresses through childhood and after reaching adulthood. Children with type 2 SMA have more severe symptoms and faster progression than people with type 3 SMA.6
Doctors usually diagnose scoliosis using a visual exam and X-rays of the spine. Signs of scoliosis include:1
- Uneven shoulders
- One shoulder blade larger than the other
- Uneven waist
- One hip higher than the other
How is it prevented and treated?
Scoliosis occurs in most people with SMA who cannot walk. Spinal management is not usually done in people who cannot sit (type 1 SMA) because of their short life expectancy. People with type 2 and 3 SMA are the most likely to receive treatment for scoliosis.5
Physical therapy is focused on delaying scoliosis. Strengthening muscles and relaxing joints can help slow the progression of scoliosis. The most common treatments for scoliosis are bracing and surgery. Spine surgery is usually delayed until after 4 years old. After that, the decision of whether to use bracing or surgery depends on the amount of curvature, the rate of progression, and effects on breathing and mobility.5
Braces that support the ribs and spine will not cure or reverse curvature. They may prevent the curvature from getting worse, but braces are mostly used to temporarily improve stability.3,5
If scoliosis progresses, surgery may be required. The most common type of surgery used is spinal fusion. In spinal fusion, doctors connect spine bones together so they cannot move freely. Rods or screws are used to hold the spine straight until the bones fuse. Unfortunately, this surgery may prevent the use of Spinraza® (nusinersen) injections around the spine. However, some simple surgical procedures can solve this issue.1,5,7
Doctors may perform other surgical techniques to delay spinal fusion surgery. One example is inserting stabilizing rods that adjust in length as children grow.5